Article Type: Short Report
Beyond dermatomyositis: Other causes of a V-shaped rash
Indira Acharya, MD1*; Carey Field, MD2; Omar Ahmed, MD2; Ashik Pokharel, MD2
1Internal Medicine, MedStar Union Memorial Hospital, Baltimore, Maryland, USA.
2Dartmouth Hitchcock Medical Center, Lebanon, New Hampshire, USA.
*Corresponding author: Indira Acharya
Internal Medicine, MedStar Union Memorial Hospital, Baltimore, Maryland, USA.
Email ID: acharyaindira99@gmail.com
Received: Jan 10, 2025
Accepted: Feb 05, 2025
Published Online: Feb 12, 2025
Journal: Annals of Medical Case Reports and Reviews
Copyright: Acharya I et al. © All rights are reserved
Citation: Acharya I, Field C, Ahmed O, Pokharel A. Beyond dermatomyositis: Other causes of a V-shaped rash. Ann Med Case Rep Rev. 2025; 1(1): 1001.
Case presentation
A 62-year-old male from northern U.S., with a medical history of dermatomyositis, psoriatic arthritis and drug induced lupus was evaluated for acute onset of neck pain and rash on neck and upper chest for 2 weeks.
Regarding his dermatomyositis, it was diagnosed in 1990 and was successfully treated with a tapering dose of steroid with last flare occurring in 2000. His psoriatic arthritis was initially treated with adalimumab which was later switched to secukinumab after he developed severe drug induced lupus in context of TNF inhibitors.
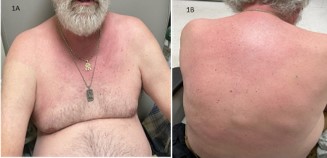
The patient described his neck pain as constant, burning type, radiating down towards bilateral shoulder joint and aggravated by any movement. He denied recent trauma, morning stiffness, upper extremity weakness, fever or any recent change in medications. The neck pain did not improve with ibuprofen. Concurrently, he noticed erythematous, non-pruritic rash in anterior neck and chest, which eventually spread to his upper back (Figure 1A & 1B). He attributed his symptoms to prolonged involvement in berry picking 2 weeks ago.
On presentation, he was afebrile and normotensive, with a blood pressure of 124/78 mmHg and a heart rate of 82 beats per minute. Physical examination showed nontender, erythematous rash in anterior neck and chest involving bilateral shoulder joint and upper back, no increased warmth of overlying skin, restricted range of motion of neck, mainly on anterior and lateral flexon.
MRI cervical spine without contrast demonstrated degenerative changes at C5-C6 resulting in severe neuroforaminal narrowing on the right and mild neuroforaminal narrowing on the left. Central focal posterior disc oetophyte complex and hypertrophy of ligamentum flavum results in moderate to severe central spinal canal stenosis.
Laboratory findings
| WBC: 6800 cells/microlitre (reference range: 4500 – 11000 cells/microlitre) |
| Lyme testing negative |
| AST: 12 U/L (reference range: 8-33 U/L) ALT: 16 U/L (reference range: 4-36 U/L) |
| Creatine kinase: 140 unit/L (reference range: 0-160 unit/L) |
| CRP: 6 mg/L (reference range: <=4.9 mg/L) ESR: 28 mm/hr (reference range: 0- 20 mm/hr) |
| Negative: SSA, SSB, smith ab, RNA polymerase 3, Jo-1 ab, PL-7 ab, PL-12 ab, EJ ab, SRP ab, MI-2 ab, MDA ab |
| C3: 145 mg. dL (reference range: 90-180 mg/dL) C4: 28 mg/dL (reference range: 10-40 mg/dL) |
| Aldolase: 12.1 U/L (reference range <=8.1) |
Discussion and further course
This patient initially presented with neck pain and a rash on his anterior neck and chest, which later progressed to his upper back. He did not experience muscle pain or weakness, fever, joint swelling, or fatigue. Given his history of prior drug-induced lupus and dermatomyositis, these conditions were under consideration. Since his symptoms began after berry picking, other differential diagnoses included allergic contact dermatitis, insect bites, and photodermatitis.
In the absence of any recent changes in his medications, drug-induced lupus was considered unlikely. Given the sparing of his hands and forearms by the rash, contact dermatitis secondary to berry picking was also less likely. Additionally, the absence of silvery-white scales in the rash and the lack of involvement of other joints made a flare of psoriatic arthritis less likely. While the presence of a rash on the sun-exposed anterior chest suggested a photosensitive rash, the involvement of non-sun exposed areas such as the back, along with the absence of itching—features not typical of polymorphic light eruption—made that diagnosis unlikely. Given his prior history of dermatomyositis, it remained high on the differential, especially considering the pattern of the rash, which resembled the shawl sign of dermatomyositis. However, a rash secondary to an insect bite could not be ruled out.
The patient underwent a punch biopsy of the skin rash, which revealed a perivascular and periadnexal inflammatory infiltrate extending into the deep dermis, composed of atypical lymphocytes and plasma cells, consistent with erythema migrans. The biopsy did not show the perivascular predominance of CD4+ T lymphocytes or interface dermatitis,which are characteristic of dermatomyositis. Repeat Lyme testing for IgG and IgM antibodies returned positive results.
Lyme disease is a systemic illness caused by the spirochete Borrelia burgdorferi, typically transmitted through the bite of the deer tick Ixodes scapularis [2]. Erythema migrans is the most common early manifestation of Lyme disease, appearing 3 to 30 days after the tick bite in 50% to 83% of cases [3]. The rash may be accompanied by systemic symptoms such as fever, fatigue, malaise, arthralgia, and myalgia in 50% of patients [1,2]. The rash is typically annular with homogenous erythema ranging from 5 to 68 cm in size and may present in various patterns, such as central erythema (59%), central clearing (30%), or central purpura (2%) [3].
The diagnosis of Lyme disease is based on characteristic clinical features in patients who live in or have recently traveled to an endemic area. In the early stages of infection, serologic tests are often negative, with only 20% to 40% of cases showing IgM seropositivity for B. burgdorferi [2]. In atypical cases, a skin biopsy may be performed to rule out other conditions. Histopathological examination usually shows a superficial and deep perivascular lymphocytic infiltrate, with plasma cells located at the periphery of the lesion and eosinophils in the center [2].
Lyme disease is generally treated with a 3 to 4-week course of oral doxycycline, amoxicillin, or cefuroxime axetil [3]. In our patient, symptoms fully resolved following a 3-week regimen of doxycycline. Although the rash of dermatomyositis can resemble erythema migrans, the absence of other key features, such as progressive proximal muscle weakness and elevated creatine kinase levels, makes dermatomyositis unlikely in this case.
References
- Nadelman RB. Erythema migrans. Infectious Disease Clinics. 2015; 29: 211-39.
- Wilson TC, Legler A, Madison KC, Fairley JA, Swick BL. Erythema migrans: a spectrum of histopathologic changes. The American Journal of Dermatopathology. 2012; 34: 834-7.
- Feder Jr HM, Abeles M, Bernstein M, Whitaker-Worth D, GrantKels JM. Diagnosis, treatment, and prognosis of erythema migrans and Lyme arthritis. Clinics in dermatology. 2006; 24: 50920.