Article Type: Case Report
Jejuno jejunal intussusception presenting as recurrent left iliac fossa pain
Samitha Senevirathne*; Jayamini Kaushalya; Anjana Abeysinghe; Albert Joseph; Ishan De Zoysa
University Surgical Unit, National Hospital of Sri Lanka, Colombo, Sri Lanka.
*Corresponding author: Samitha Senevirathne
University Surgical Unit, National Hospital of Sri Lanka, 19/1A, Thilaka Road, Gampaha 11870, Colombo, Sri Lanka.
Received: Jan 20, 2025
Accepted: Feb 12, 2025
Published Online: Feb 19, 2025
Journal: Annals of Medical Case Reports and Reviews
Copyright: Senevirathne S et al. © All rights are reserved
Citation: Senevirathne S, Kaushalya J, Abeysinghe A, Joseph A, De Zoysa I. Jejuno jejunal intussusception presenting as recurrent left iliac fossa pain. Ann Med Case Rep Rev. 2025; 1(1): 1003.
Abstract
Intussusception occurs as a result of invagination of a proximal bowel segment into immediate adjacent distal bowel segment. This can occur with or without the presence of a lead point and occur between different anatomical regions of bowel. Paediatric and adult intussusception are different to each other in terms of symptomatology, aetiology and management. Here we have described a 48-year-old male who has been evaluated for recurrent left iliac fossa pain presenting with intestinal obstruction diagnosed with jejuno jejunal intussusception and the subsequent management. Considering the complications associated with the adult intussusception and the possibility of a malignant aetiology, the clinicians should have a high degree of suspicion to improve patient outcomes although it’s a rare entity.
Keywords: Intestinal obstruction; Intussusception; Smal bowel resection.
Introduction
Intussusception is a condition caused by invagination of a bowel segment into its adjacent segment which is also called telescoping. It is common in paediatric population with a peak incidence at the age of 5-7 months [1]. It’s relatively uncommon in adult population. The typical symptoms include colicky abdominal pain, blood and mucus-tinged stools and vomiting [2]. It accounts for 1% of adult intestinal obstruction [3]. Telescoping is triggered by increased peristaltic activities at a transition point. Even though paediatric intussusception is predominantly idiopathic due to lymphoid hyperplasia following viral infections, 90% of the adult intussusception will have a pathological lead point [4]. This process can occur in between large bowel segments, small bowel segments and small and large bowel segments. We present a patient with jejuno jejunal intussusception caused possibly by an intestinal lipoma presenting with intestinal obstruction. Informed consent was obtained from the patient for anonymized reporting of details.
Case presenation
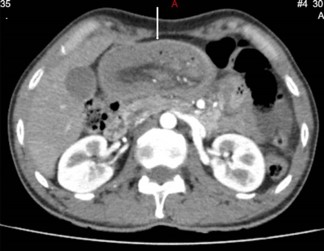
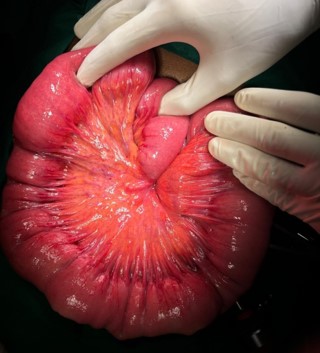
A 48-year-old otherwise healthy male presented to national hospital of Sri Lanka in September 2024 with a complaint of intermittent left iliac fossa pain for 6 months duration. The pain was colicky in nature which lasts for about 10 minutes. This was associated with loss of appetite and loss of weight of 6kg over a period of 4 months. He also complained of constipation predominant altered bowel habits for the same duration. He has never had per rectal bleeding. During this period the patient has had multiple hospital admissions in which he has been managed with the suspicion of diverticular disease and ureteric colic. However, he has never had episodes of intestinal obstruction. He has never had previous abdominal surgeries as well. During these admissions he has been evaluated with upper and lower gastrointestinal endoscopy and ultrasound scan of the abdomen which did not show any remarkable finding. In this admission he complained of similar type of abdominal pain with bilious vomiting and absolute constipation for 4 days duration. On examination he had a soft distended abdomen with an empty rectum in the digital rectal examination. He was neither febrile nor tachycardic. The blood investigations were unremarkable. It was decided to proceed with contrast enhanced CT of the abdomen which showed evidence of telescoping of the jejunal loops with the lead point in the mid jejunum (Figure 1). CT abdomen further showed a submucosal fat density in mid jejunum which is likely to be an intestinal lipoma which could be the lead point. Since the patient has been having recurrent episodes and considering the chance of adult intussusception having a lead point which will predispose the patient for future intussusception, it was decided to proceed with diagnostic laparoscopy with or without laparotomy. The diagnostic laparoscopy revealed a dilated proximal jejunal loop with thickened bowel wall. No lead point was noted macroscopically. As the laparoscopic handling of the bowel mass was difficult, the procedure was converted to open laparotomy. The dilated thickened bowel segment was resected and side to side jejuno jejunal anastomosis was done (Figure 2). The patient had an uneventful postoperative recovery and discharged from hospital on post operative day 5 after fully establishing normal diet. The patient was reviewed with the histology in surgical clinic where no specific lead point was identified. As the histology was benign and the patient was symptom free, he was discharged from the clinic and will be reviewed if needed.
Discussion
Intussusception occurs when one part of the gut invaginates into immediate adjacent segment. The inner tube is called the intussusceptum and the outer tube is called intussuscepien [5]. Intussusception is classified as idiopathic or primary and secondary. Secondary intussusception can be caused by Meckel’s diverticulum, polyps, duplication, Henoch Schonlein purpura in children and adenocarcinoma, peritoneal metastasis, adhesions, trauma in adults [6,7]. Depending on the site of the intussusception, it can be classified as enteric, ileocolic and colocolic and they account for 49.5%, 29.1% and 19.9% for adult intussusception respectively [8]. Out of these three types 22.5%, 36.9% and 46.9% occur in a background of malignancy respectively. Out of the malignant causes majority of enteric intussusception is associated with metastatic adenocarcinoma while ileocolic and colocolic intussusceptions are associated with primary adenocarcinoma. This can be complicated with intestinal obstruction, bowel ischaemia, perforation, peritonitis and lifethreatening sepsis.
Multi Detector Computer Tomography (MDCT) is considered as the best modality to diagnose intussusception with a reported accuracy of 60-100%. It can diagnose intussusception, presence or absence of lead point and the associated complications. Target sign, reniform bilobed appearance and the sausage shaped appearance are the commonest characteristic appearances [9].
Optimal management of adult intussusception remains a controversy where the debate is centred between reduction vs resection. Although reduction techniques like hydrostatic reduction and pneumatic reduction are described for paediatric intussusception, reduction is not recommended for adults due to high chance of failure and hypothetical risk of dissemination of malignancy and perforation [10]. As the presence of malignancy as the lead point is high in ileocolic and colocolic intussusception, resection without reduction is advocated. Although not convincing as for colocolic intussusception, the risks associated with reduction still apply to enteric intussusception as well. The only theoretical benefit appears to be the preservation of bowel length. The combined endoscopic and laparoscopic approach has been suggested without resection for patients with intestinal polyposis syndromes with recurrent intussusception to preserve the bowel length [10,11].
In our patient who presented with possible recurrent enteric intussusception probably misinterpreted as diverticular disease or ureteric colic underwent small bowel resection. Although it was preoperatively identified that the lead point is benign, reduction was not attempted considering the age, history of multiple episodes and the risk of iatrogenic bowel perforation associated with reduction.
Conclusion
The jejuno jejunal variant of adult intussusception is a rare entity that a surgeon would come across only a handful number of cases during his career. Although rare, if not timely detected, this can lead to life threatening complications or long term poor oncological outcomes. The diagnosis would be made further difficult by the non-specific symptoms and presence of other common differential diagnosis. Therefore, clinicians should have high index of suspicion to not to miss intussusception. Computed tomography remains the mainstay of diagnosis, with surgical resection being the mainstay of management.
Declarations
Conflicts of interest: The authors declare no conflicts of interest. The study received no funding from any third party.
References
- Boucher B, Fleites O, Varghese R, Myuran Nagaratnam J, Yabit F, Jorge J. Intussusception in the Geriatric Population: A Case Report. Cureus. 2022; 14: e24663.
- Yalamarthi S, Smith RC. Adult intussusception: case reports and review of literature. Postgrad Med J. 2005; 81: 174-7.
- Shaheen K, Eisa N, Alraiyes AH, Alraies MC, Merugu S. Telescoping intestine in an adult. Case Rep Med. 2013; 2013: 292961.
- Hadid T, Elazzamy H, Kafri Z. Bowel Intussusception in Adults: Think Cancer! Case Rep Gastroenterol. 2020; 14: 27-33.
- O’Connell PR, McCaskie AW, Williams NS. (Eds.). Bailey & Love’s Short Practice of Surgery, 27th Edition (27th ed.). CRC Press. 2018.
- Lu T, Chng YM. Adult intussusception. Perm J. 2015; 19: 79-81.
- Marinis A, Yiallourou A, Samanides L, Dafnios N, Anastasopoulos G, et al. Intussusception of the bowel in adults: a review. World J Gastroenterol. 2009; 15: 407-11.
- Hong KD, Kim J, Ji W, Wexner SD. Adult intussusception: a systematic review and meta-analysis. Tech Coloproctol. 2019; 23: 315-324.
- Valentini V, Buquicchio GL, Galluzzo M, Ianniello S, Di Grezia G, et al. Intussusception in Adults: The Role of MDCT in the Identification of the Site and Cause of Obstruction. Gastroenterol Res Pract. 2016; 2016: 5623718.
- Eisen, Leon K, John D, Arthur H. Intussusception in adults: institutional review. Journal of the American College of Surgeons. 1999; 188: 390-395.
- Alonso Verónica, Ma Targarona Eduardo, Bendahan Galit Even, Kobus Christian, Moya Isabel, et al. Laparoscopic Treatment for Intussusception of the Small Intestine in the Adult. Surgical Laparoscopy, Endoscopy & Percutaneous Techniques. 2033; 13: 394-396.